A multicentre study shows that ALS patients use therapeutic movement exercisers at home intensively—5+ times a week—and report improved well-being, reduced stiffness, and an excellent Net Promoter Score of +61.

The study analysed 106 patients with ALS (women: 64%, n=68; men: 36%, n=38) who were supplied with a therapeutic movement trainer. The study was conducted from February 2019 to January 2020 at nine specialised ALS centres. Data collection with a structured interview was carried out via the management and research platform www.ambulanzpartner.de.
People with amyotrophic lateral sclerosis (ALS) suffer progressive paralysis of the arms and legs. Therapeutic movement exercisers are an aid that enable device-based physiotherapy of the legs and arms in the home. Therapeutic movement exercisers for the arms and legs offer an active or passive mode of device-based physiotherapy, depending on the severity of the paralysis.
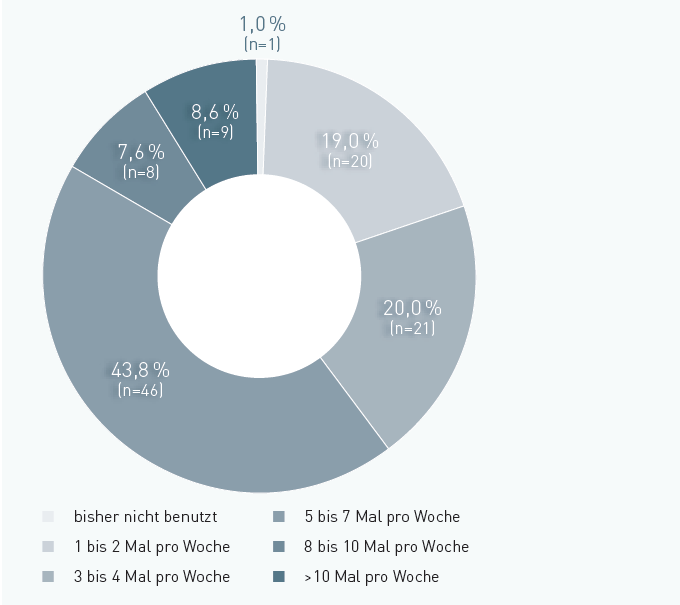
The majority of patients (60%) use the therapeutic movement exerciser at least 5 times a week. Almost 9% even get device-based physiotherapy more than 10 times a week. Only 19% use the equipment only once or twice per week. The exact weekly frequency of use is shown in the figure (Fig.1).
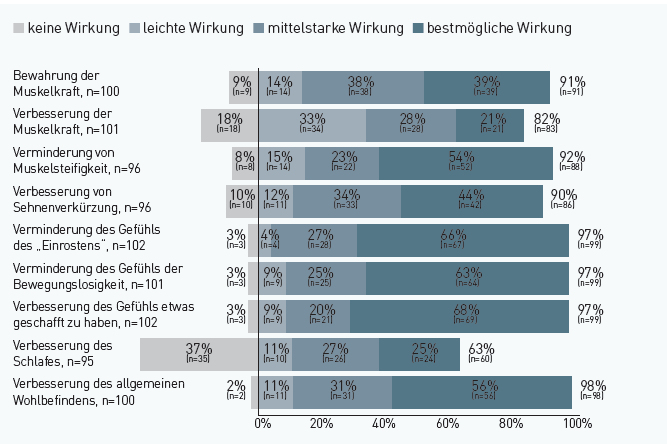
From the patients’ experiences, the following picture emerges about the benefits of therapeutic movement exercisers. Four treatment areas achieve a particularly high approval rating: Improvement of general well-being (98%), reduction of the feeling of immobility, improvement of the feeling of “having done something” and reduction of the feeling of “becoming rusty” (97% each). The two treatment goals of reducing muscle stiffness (92%) and preserving muscle power (91%) were also confirmed at high levels. Other important effects are shown in the following figure.
Satisfaction with a therapeutic movement exerciser was determined by the so-called likelihood of recommendation using the Net Promotor Score (NPS): “How likely is it that you would recommend the movement exerciser to a friend or colleague who suffers from spasticity or flaccid paresis?” The answers were given on a scale between 0 (absolutely unlikely to recommend) and 10 (highly likely to recommend) points.
The likelihood of recommendation for a therapeutic movement exerciser was assessed at an NPS of +61 points (NPS scale -100 to +100, >0 = positive evaluation). This corresponds to a very high level of satisfaction with the tool (Fig.3).
The study allows an in-depth insight for the first time into the topic of therapeutic movement exercisers for patients with ALS. The issue is particularly controversial due to the restrictive coverage of the costs of care by health insurance funds. The majority of patients with ALS (60%) use the therapeutic movement exerciser at least 5 times a week and are therefore getting frequent device-based physiotherapy in addition to their physiotherapy treatment. From the perspective of patients, the examined subjective treatment goals of device-based physiotherapy are almost universally achieved. Patient satisfaction with the therapeutic movement exerciser is very high (NPS: +61, an NPS >50 is considered “excellent”).
The study clearly demonstrates the treatment potential of therapeutic movement exercisers for ALS. So far, however, the possible applications of a movement exerciser for ALS are insufficiently known and under-communicated.
In order to further develop the treatment method, it is important to find out in future studies whether an improvement of functions (e.g. through a reduction of spasticity) can also be achieved through device-based physiotherapy. Future analyses must also show how the use of therapeutic movement exercisers affects the emergence and development of secondary symptoms of limb paralysis (pain, contractures, lymphoedema) in ALS.
We would like to thank all the patients who participated in this movement exerciser study and provided their data for research. The research project was only able to succeed thanks to their kind support and the data they provided.
• Charité - University Hospital Berlin, outpatient clinic for ALS and other motor neurone diseases
• Bergmannsheil University Hospitals, outpatient clinic for ALS and other motor neurone diseases
• University Hospital Jena, Centre for Neuromuscular and Motor Neuron Diseases
• Alfried Krupp Hospital Essen, outpatient clinic for ALS and other motor neurone diseases
• University Hospital Bonn – Clinic for Neurodegenerative Diseases
• University Medical Center Göttingen – outpatient clinic for ALS and other motor neurone diseases
• University Hospital Leipzig – outpatient clinic for ALS and other motor neurone diseases
• University Hospital Dresden – outpatient clinic for motor neurone diseases
• Diakonissenkrankenhaus Mannheim, Neurology Clinic
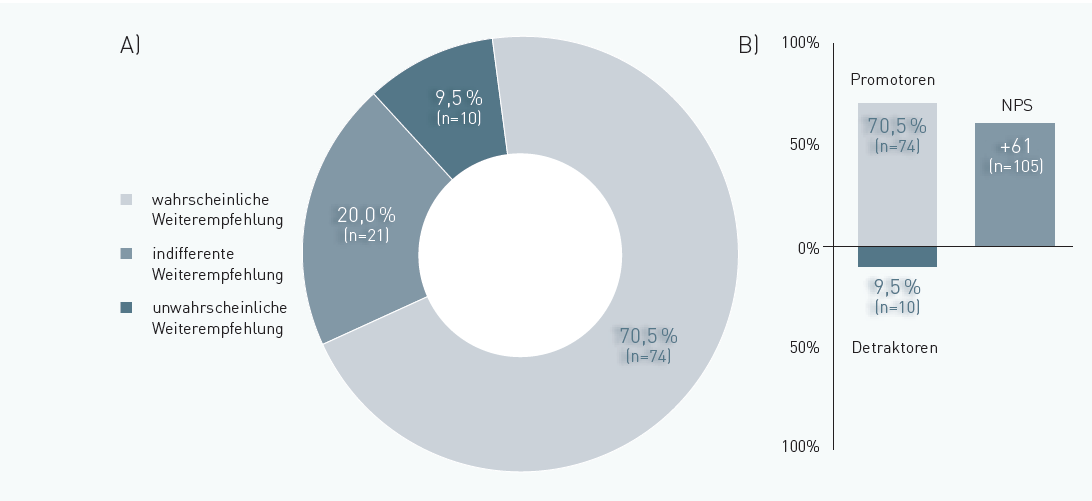

- Susanne Spittel, M.Sc. Projektleiterin medizinische Forschung Mail: susanne.spittel@ap-soziotech.de Fon: 030 81031410
Related contents
Find related exciting contents in our media library.
Meet our specialists.
Are you interested in our solutions? Schedule a meeting with a Consultant to talk through your strategy and understand how TEHRA-Trainer can help you to advance rehabilitation.
You need to load content from reCAPTCHA to submit the form. Please note that doing so will share data with third-party providers.
More InformationYou are currently viewing a placeholder content from Turnstile. To access the actual content, click the button below. Please note that doing so will share data with third-party providers.
More Information