Therapy & Practice
Early mobilisation in the intensive care unit
Early mobilisation protocols (EMP) for patients can significantly reduce length of stay in medical intensive care units and hospitals. Alongside an improved clinical outcome, there are also discussions around financial advantages, which mean that corresponding measures pay for themselves.
As part of a prospective pre-post comparison study, Klein and colleagues of the Cleveland Clinic Foundation investigated the impacts of an early progressive mobilisation protocol (EPMP) on the costs of a neurological intensive care unit. For the study, researchers recruited adult patients who were being treated at a neurological intensive care unit with 22 beds. Alongside demographic data on the patient, the data collected included medical history, the degree of severity of the illness, mobility restrictions before the hospital stay (walking aids, physical restrictions), use of ventilators, the duration and reintubation, and direct, indirect and overall hospital costs. 637 patients on the neurological intensive care unit met the inclusion criteria. The average age was 62 (+/- 16) years. The APACHE III score for the severity of the illness was 57 points (+/- 27), indicating an illness of moderate severity.
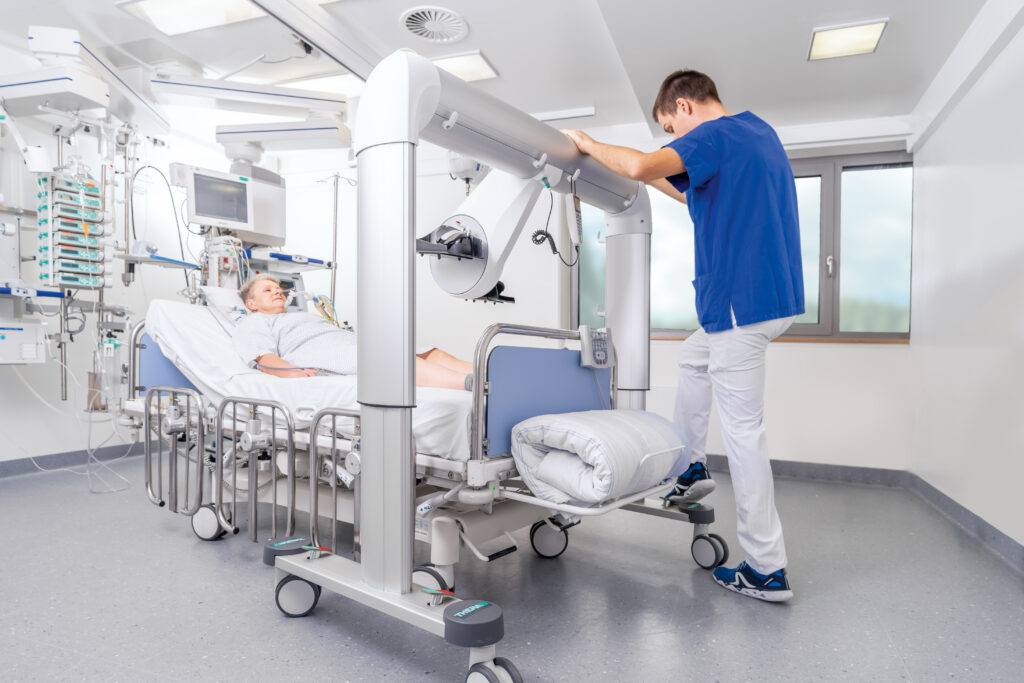
The percentage of patients requiring mechanical breathing assistance was lowered by the use of an early progressive mobilisation protocol by 15% (before EPMP, 48.5% and after EPMP, 33.7%, p < 0.001), and the number of days on ventilation was reduced by 51% (before EPMP, 3.5 days compared to 1.5 days after EPMP, p < 0.001).
The cost analysis data included 605 individual hospital stays (30 had several stays on the neurological intensive care unit and no cost data was available for 2), meaning 603 cases were analysed (before EPMP, n = 221 and after the EPMP, n = 382). After adjustment for the demographic baseline data of the patients, which was different between groups (walking aid and gait disorder), the average direct, indirect and overall costs post EPMP fell by 30% (+/- 1%) compared to pre EPMP (p < 0.001).
The introduction of an EPMP in the neurological intensive care unit led to a reduction in overall hospital costs. The verifiable cost savings can be used to purchase safe patient handling equipment to improve the safety of caregivers, therapists and patients. The results increase the transparency of decisions on the allocation of funds for the introduction of early mobilisation protocols and help to make the underlying decision criteria explicit.
Jakob Tiebel
Related contents
Find related exciting contents in our media library.
Meet our specialists.
Are you interested in our solutions? Schedule a meeting with a Consultant to talk through your strategy and understand how TEHRA-Trainer can help you to advance rehabilitation.