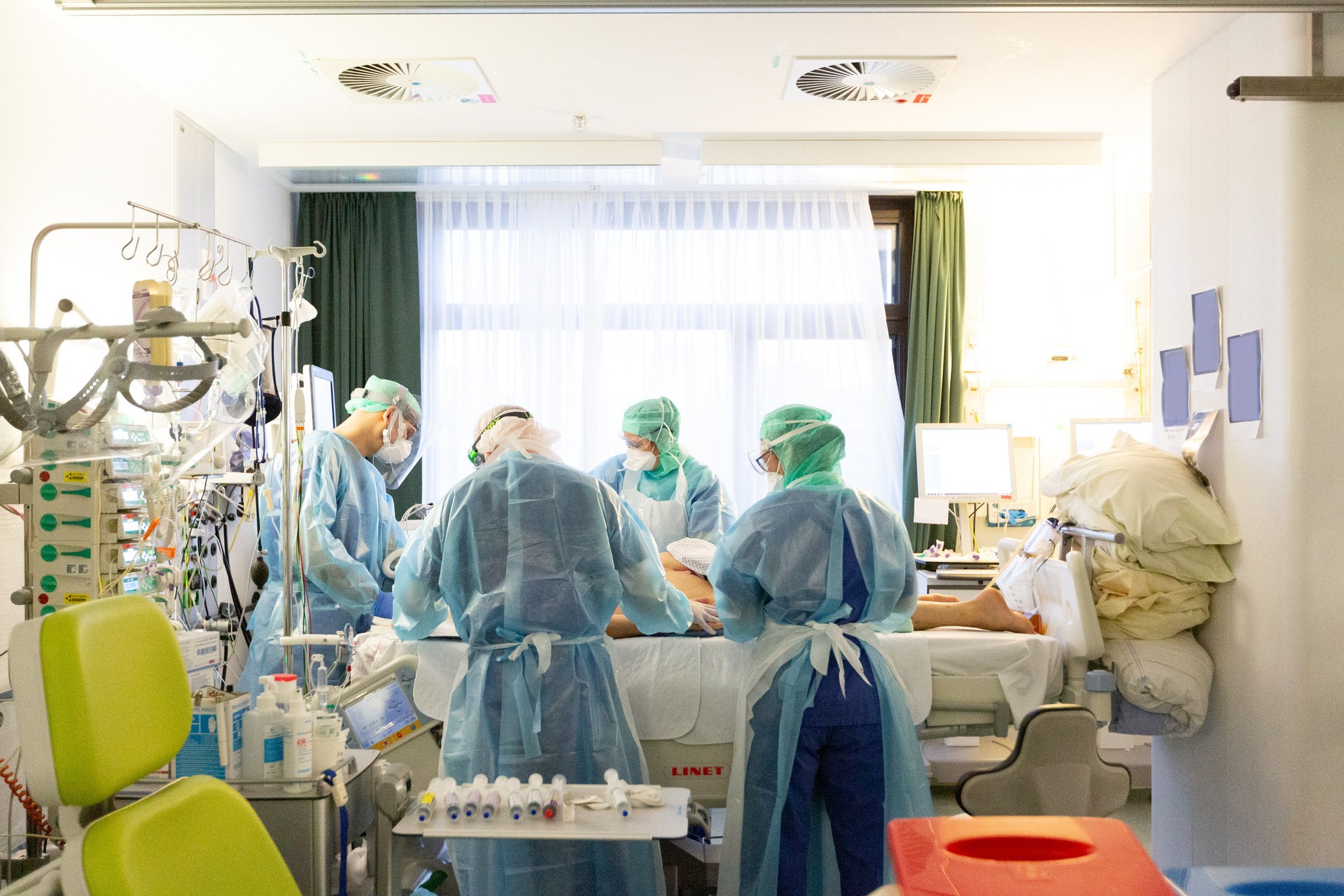
Discover how physiotherapists on intensive care units support Covid-19 patients with early mobilisation, respiratory therapy, and close interdisciplinary teamwork—insights from Tübingen University Hospital.

Editorial: Thank you for agreeing to do this interview, Tobias. You’re a physiotherapist at Tübingen University Hospital. What is the current Covid situation from a physiotherapy perspective?
Tobias Giebler: I can answer this question specifically for the area of intensive care units. In any case, it must be said here that it is a huge interdisciplinary challenge to implement early mobilisation.
How does it work? Together, the patient and the situation are considered. Therapy options are evaluated taking into account the latest findings, and treatment goals and priorities are set. If possible, the patient is involved at this stage. It’s important to know that Covid patients are kept in the prone position for 16 hours a day while the lungs are still massively affected. Then they are turned back to the supine position and sedation is reduced as much as possible. Patients should be awake and if there are no contraindications, this phase is then used for mobilisation. If a break from sedation is not possible, our only options are respiratory therapy in bed in different starting positions, and passive movement of the patient. Most of the time, these are severely affected patients. Not only the lungs, but many other organs, such as the central nervous system, the kidneys, the liver and the intestines are affected. As a result, the patients have many inputs and outputs, such as ventilation, infusions, possibly ECMO cannulas (extracorporeal membrane oxygenation, “artificial lung”) and dialysis tubes. Offering an adequate therapy programme to cardiopulmonary unstable patients is challenging. We have to be incredibly vigilant and attentive. We’ve also found over the past two years that managing exercise intensity in these patients is a challenge. The condition and prerequisites associated with it change quickly. It’s important that we do not overburden them in any way. Metabolism seems to be very catabolic in Covid patients. They lose muscle mass quickly and strongly, so they need a lot of support from us. For this reason, we are mainly dealing with severely affected adynamous patients who demand maximum attention in early mobilisation and respiratory therapy. What makes it even more difficult for us is that the whole intervention takes place in full PPE. You sweat and quite often find you have limited vision due to fogged up protective goggles – an exhausting undertaking.
Tobias Giebler: This is a really complex and personal question. Especially in the early days, when we didn’t know exactly what we were dealing with, it was incredibly stressful. No one knew how the situation would develop or how well your own family would be protected. Uncertainty was a constant companion during this time. In addition, we were shown again and again how the situation presents itself and can develop, that the general condition of these people who are affected can deteriorate massively in a short time and sometimes they also die. Being constantly confronted with the topic of death, even in young, previously healthy people, was and is a burden. Even without Covid, we are dealing with severely affected patients and tragedies in the intensive care unit.

Tobias Giebler: Since I don’t work in this field, I can’t answer this from my own experience.
Editorial: If we look back at the patient and go even deeper here, what are the focal points in the physiotherapeutic activity but also in the interdisciplinary cooperation with the other professional groups that work with the patient? What are the interventions that you do?
Tobias Giebler: Physiotherapy is divided into three pillars here. One pillar is early mobilisation from the first exercises in bed to gait training. This often takes place under ECMO therapy. We know that early mobilisation, with its many positive effects, has a huge influence on the development of complications, the length of stay in the intensive care unit and, most of all, on the outcome. Respiratory therapy, the second important pillar, is usually integrated into early mobilisation. Here, our experience is that in Covid patients we need to look at maintaining thoracic mobility and lowering breathing resistance to improve breathing work over tissues and muscle techniques. On top of this, reducing the coughing stimulus is an issue. We take care of secretion in the lungs and the management around it. This also includes various positions that help to improve the ventilation-perfusion ratio in the lungs. We treat ventilation disorders (atelectasis/dystelectasis) and try to prevent them. While doing this, we then support the weaning process – and by that I mean the path of weaning from ventilation and ECMO therapy. We strengthen the respiratory muscles and then work to help patients learn to breathe again as effectively as possible and reacquire a physiological breathing pattern. This is a particular issue for those with Covid disease. Again and again it seems as if the patients have forgotten how to breathe physiologically, as if their central coordination has also been affected. Finally, the third pillar is mental support, the psychological aspect. You have to realise that the patients are in an extreme state of emergency. Visits are only possible to a limited extent; at the beginning of the pandemic visiting was not allowed at all. We become the patients’ close confidant and contact person, because we spend a lot of time with them.
Editorial: A summary of all these descriptions: What are the biggest challenges in working with patients who have Covid-19?
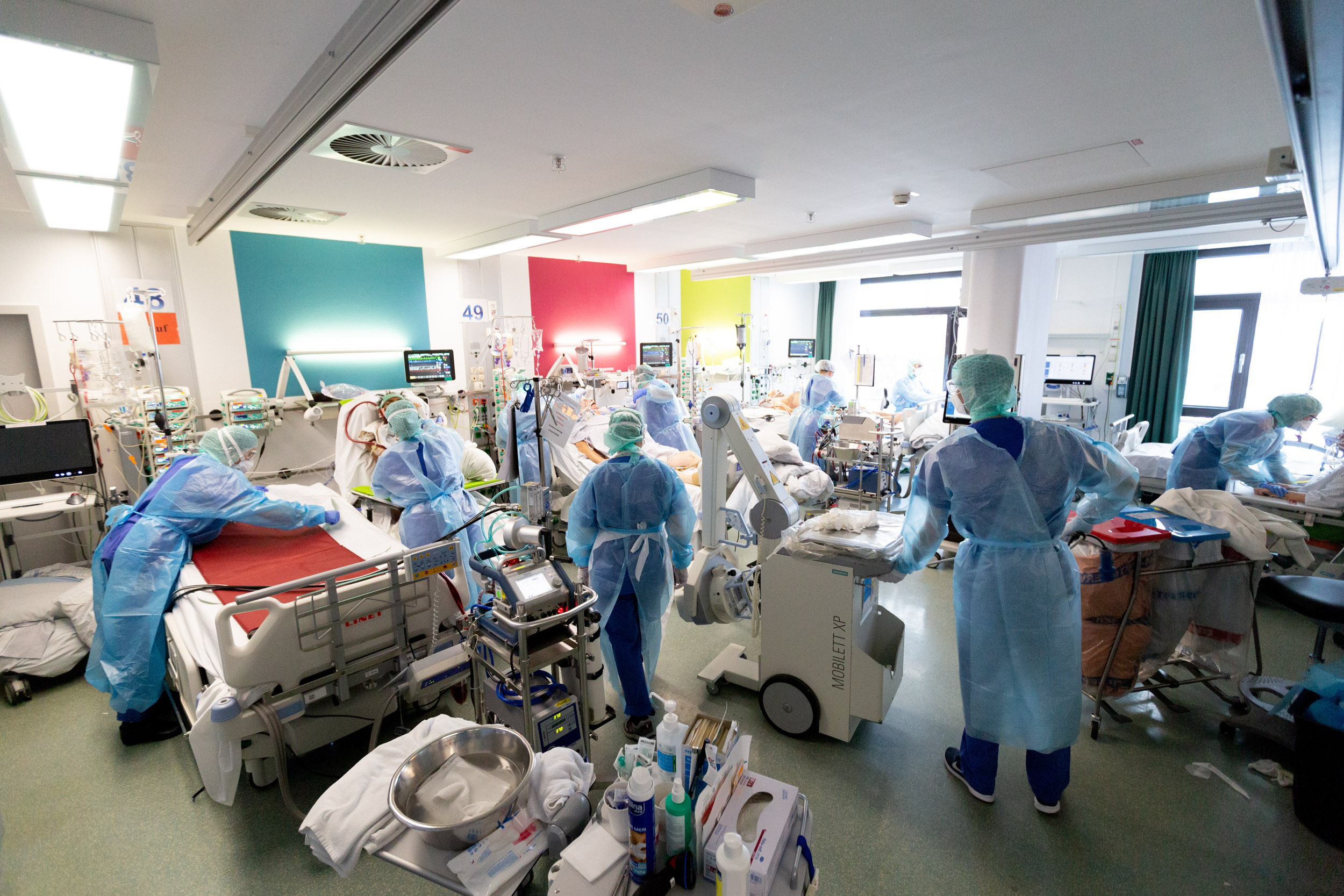
Editorial: In conclusion: Do you maybe have a nice or positive anecdote from everyday life?
Tobias Giebler: Time and again, we also have patients who are particularly memorable and stories that are especially touching. For example, I just remember a pregnant patient who came to us in the intensive care unit. It became clear that the patient needed ECMO therapy and and the baby had to be delivered as early as 28 weeks gestation. This woman was lying with us and was badly affected. Finally, after about 7 weeks, she was able to walk a few steps again and sit in a wheelchair regularly.
What she wanted most of all and what motivated her daily to keep at the hard struggle back into mobility was to see her child for the first time. From the intensive care unit, it was organised that an ambulance with incubator went to the neonatology unit and together with a paediatrician the baby was brought to us in the intensive care unit. The overjoyed mother and her child could then be reunited in a separate room. These are moments that everyone can naturally draw a lot of energy from!
Editorial: Thank you for this exciting insight!

Related contents
Find related exciting contents in our media library.
Meet our specialists.
Are you interested in our solutions? Schedule a meeting with a Consultant to talk through your strategy and understand how TEHRA-Trainer can help you to advance rehabilitation.